Hydrotherapy Myths
Myth 1: Aquatic Therapy Cannot Happen Until A Wound Is Healed
“Aquatic therapy can’t begin until a wound is completely healed…right?”
This statement is uttered on a regular basis, usually by well-meaning professionals who are unaware that it’s based on antiquated understandings and misconceptions about water therapy.
Randy Cohen of the University of Arizona is no stranger to physical therapy and athletic training, having received his degrees from Purdue University and the University of Illinois-Chicago. He’s been with the University of Arizona since 2001, and maintains an excellent reputation for using aquatic therapy as early as one week post-op to help the athletes under his supervision begin to actively heal. Not only are many of those athletes still on crutches when they begin to work with Cohen, but they also have wounds that haven’t scabbed over, and/or stitches that haven’t been removed.
How does Cohen make sure they are able to safely get in the water? His trick is hardly magic – it’s just a purely pragmatic, proven waterproofing technique.
- The process to waterproof a wound that has stopped draining (and isn’t infected) but isn’t completely healed takes only a few moments, surprisingly:
- Expose the wound and remove any current dressings.
- Make sure the area around the wound is completely dry.
- Cut a piece of gauze pad to fit over the wound. The gauze will be used later to document that the wound was kept dry throughout the aquatic therapy session.
- Spray the area around the wound with stick-it to provide stronger skin anchoring for the next step.
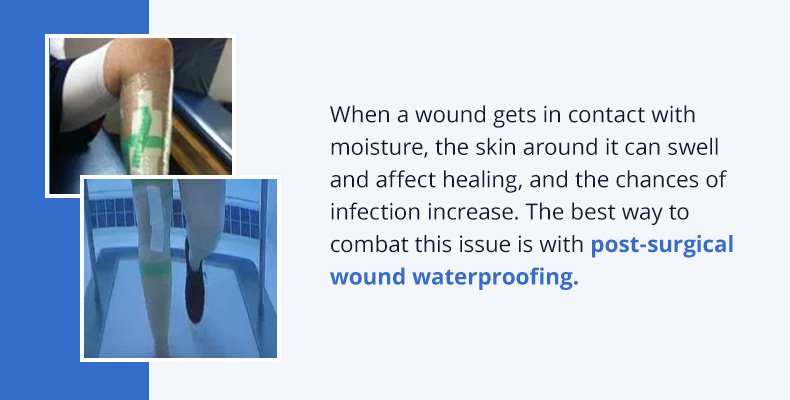
- Completely cover the wound and gauze with a bioclusive clear waterproof dressing, pushing and rubbing it down along the edges until it is smooth. The dressing should be big enough to seal the wound; some athletic trainers and physical therapists prefer to double-up by placing two dressings on the site for added security.
- If the area is not a joint Flex Wrap can be used around the extremity to create an extra waterproof barrier.
At this point, the dressing should be checked to make certain that it stays in place without hindering movement. For instance, if the wound is along a joint such as the knee, the athlete or patient should bend and extend the knee several times to ensure that the seal of the bioclusive dressing doesn’t break. As long as the wound can’t get wet, it’s fine to proceed with the aquatic therapy session!
In fact, Cohen has never – and we mean never – had one of his athletes get an infection or experience wound dehiscence (i.e., the rupturing of stitches) because of early aquatic therapy intervention.
Of course, physicians tend to be conservative by nature, so it may take a little convincing to assure them that a patient with an unhealed, but no longer draining, wound can start physical therapy in the pool. In Cohen’s experience, when doctors see the documentation that the gauze pad (in step three, above) always stays completely dry, they tend to become more comfortable with allowing aquatic therapy within the first few weeks post-op.
Myth 2: Aquatic Is Limited To Rehab
As Lance Walker of Michael Johnson Performance has noted, any professional who is limiting aquatics to only rehabilitation needs to “wake up and smell the bacon,” because this limitation is definitely considered “old school.”
Today, trainers, athletes, coaches and exercisers are all using therapy pools as modalities to cross-train without putting major stressors on the body. For instance, throughout the United States, most professional athletic teams and colleges with high-profile sports teams have at least one HydroWorx pool at their disposal, and Walker says with confidence that they definitely use those pools for more than rehab.
Yes, they use their therapy pools for rehab if a player is on the injured list, but they also use the pool as a secondary training modality. Even Olympians are regularly getting in the water to increase their strength and endurance without hurting their bodies.
Myth 3: You Can’t Match Land Running In Water
Walker commonly works with his athletes in the pool, focusing on plyometrics, dynamic mobility, reactive footwork and much more. As a tool, the therapy pool provides the efficiency and effectiveness Walker’s clients need to improve their performance (and potentially make more money in the case of pro athletes).
So how does this work from an evidence-based perspective? The key is to make use of all the pool functions. By turning on the high-powered resistance jets and/or increasing the speed on the underwater treadmill, it’s possible to foster an environment where high intensity is the name of the game. However, there’s no pounding of the joints, which makes an intense conditioning pool workout perfect for adding training hours without risking injury. Recent research from Utah State University further validates this truth. The researches conducted the study, “Metabolic Cost Comparison of Running on an Aquatic Treadmill with Water Jets and Land Treadmill with Incline,” to compare the metabolic costs at specific inclines while running on a land based treadmill to running speeds on an aquatic treadmill with the resistance jets. And the study concluded that running on an underwater treadmill against the resistance jets results in a greater change in metabolic cost than running on a land based treadmill.
Myth 4: It Is Impossible To Replicate Land Running or Walking Gait In The Water
Science has now proven, thanks to stop-motion videos, that it is absolutely possible to replicate land movements in the water. The key is to equip the therapy pool with an underwater treadmill, whereby it’s easy to examine an athlete’s movements via an underwater camera.
By studying the hip, knee and leg angles appropriate for healthy land-based running or walking, not to mention foot strike tendencies, athletic trainers, physical therapists and strength coaches can help their clients mimic those movements in the pool. Not only will the movements then translate to land, but the stressors on other parts of the body will be lowered. Plus, there’s no awkward transition of different movements between the land and the water; the athlete is improving and perfecting his or her natural gait whether in the pool or on the track.
Myth 5: As Seniors Age, They Cannot Gain Muscle
One of the biggest myths that we’ve all heard is that as seniors age, it’s impossible to continuously gain muscle and strength. This myth may lead aging adults to limit themselves, which is unfortunate. Some of the most amazing athletes we’ve met are those who are eligible for AARP membership.
This misconception has been debunked, especially when considering the cases of GeriAthletes (those who are still competing in the sports they love well into their 60s, 70s, 80s and beyond.) Mike Studer, PT, MHS, NCS, CEEAA, CWT, CSST, President and Co-Owner of Northwest Rehabilitation Associates, recently presented the webinar, “GeriAthletics: Training Competitive Athletes Over 65 with High Intensity Underwater“, which was devoted entirely to this topic and helped to provide insights into debunking this myth.
Evidence based research on aging from such well-regarded organizations as the American College of Sports Medicine shows that although there are some factors that do have to be considered when building strength and gaining muscle during the senior years, both young and old populations have the same general responses to:
- Recruitment and motor learning
- Synchronization and motor control
- Fiber hypertrophy and increased muscle mass
So what’s the biggest difference for the geriathlete who wants to build muscle? It all boils down to working with the realities of aging. The aging process naturally creates an environment where the body tends to decrease muscle fiber size, decrease muscle mass and decrease bone mineral density. Our bodies respond uniquely at the cardiovascular, tendon and muscular levels. Additionally, we have a reduced capacity to clear protein, varied (and perhaps unpredictable) hormone levels, lowered capacity to repair and lessened sleep quality.
But all is not lost! To combat these factors, geriathletes participating in activities such as long-distance running, cycling, golfing and swimming are choosing to complement their land-based training regimens with regular warm water therapy exercising.
In a therapy pool with an underwater treadmill, geriathletes can focus on injury prevention, optimal performance training and maximized recovery time, all leading to plenty of benefits, including the increase of muscle mass. For instance, the hydrostatic force of the water naturally causes a positive return of the blood back to the heart, which is something that tends to diminish as the years tick by. Thus, a workout in the water mitigates some of these losses. This then promotes greater exchange and efficiency, enabling the body to load red blood cells back through the blood stream. The upshot? Muscles are supplied and stimulated, rather than quickly depleted.
Even senior athletes who have had physical problems and surgeries can gain muscle mass thanks to endurance and high intensity interval training in the pool. Effective exercises include bounding, jogging, jumping, shock drills, box sets and running against the resistance forces of high-powered jets. The buoyancy of the water helps offset impact absorption, giving a boost to the geriathlete without risk of physical harm.
Myth 6: Hydrotherapy Is Only For Lower Extremity Physical Therapy
One of the biggest misconceptions in the field of aquatic therapy is the persistent belief that therapy pools can only help patients who require treatment of their lower extremities. The foundation of this myth is easy to understand- people take one look at a four foot deep pool and picture an individual walking in it. Naturally, this means the patient is merely working his or her lower body, walking on the underwater treadmill and doing leg-related exercises. Yet this initial assumption totally misses the mark on all the ways that the pool can benefit those who require upper extremity physical therapy .
To give some background on the myth, as well as to totally debunk it once and for all, we turned to Veronica Paquette, PT, ATRIC, PRT, physical therapist and owner of the Vermont-based Essex Aquatic & Rehab Center. Veronica’s been a huge proponent of aquatic therapy for 15 years. However, when she first began working in aquatic environments, she too fell prey to the idea that she had to limit her aquatic patients to those with lower extremity issues.
Over time, though, she realized that with a bit of creativity and an open mind, her HydroWorx therapy pool could be the ideal resource for those recovering from conditions affecting their shoulders, arms, elbows, upper spine area and more. At her facility, she regularly treats people recovering from such conditions as rotator cuff tendonitis, rotator cuff repairs, shoulder replacements, shoulder impingement, elbow tendonitis and carpal tunnel syndrome.
So how does she get their upper extremities moving in the water? Check out some of these fantastic exercises she uses to speed up their healing process and get them back to a normal lifestyle as quickly as possible:
- Standing upright and leaning against the HydroWorx pool, the patient can begin to move his or her arms to the front and the sides. The water creates a bit of resistance.
- Standing away from the wall of the pool, the patient can begin to work on balance and stability exercises, such as squatting and using the upper extremities to stay in one place. With the resistance jets turned on, this can be quite effective!
- Lying in a supine (face-up) position while wearing a supportive lumbar belt, the patient can freely move his or her partially-submerged upper body. The aquatic physical therapist is also able to assist using manual techniques. Horizontal abduction and adduction exercises in this position encourage movement from the toes to the neck.
- Lying in a prone (face-down) position in the water while using a snorkel and mask, the patient can relax and allow his or her shoulders to move freely. As long as the patient is comfortable putting his or her face in the water, this position usually becomes a favorite activity during aquatic therapy sessions.
Of course, this is but a snippet of the multitude of upper extremities exercises possible in a HydroWorx therapy pool. The key is for physical therapists to be innovative in an effort to provide an adjunct to, or substitution for, more traditional land-based therapy modalities.


It’s encouraging to see so many options for joint pain relief. I’m excited to try some of these tips and improve my quality of life!