Every physical therapist will admit that there is a psychological component to patient success when it comes to returning to activity after surgery. Patients with a positive outlook and experience will exhibit more willingness to push themselves than those who have a pessimistic approach to physical and occupational therapy. One of the main barriers to optimism is the feeling of pain or discomfort. As we have found, even the expectation of pain can lead individuals into a cycle of fear avoidance. Early aquatic therapy may be one of the most reliable ways to help people avoid a downturn in their outlook after surgical procedures such as total knee replacement, back/spine surgery and hip replacement.
The Fear Avoidance Model
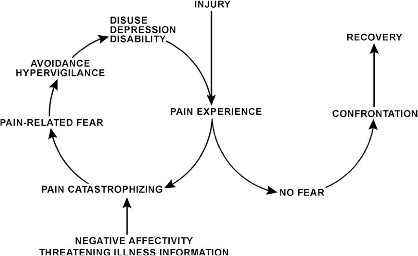
The fear avoidance model as illustrated shows what can happen when patients become trapped into thinking that they will have to experience pain if they take a certain action, such as attend physical therapy. Because they have felt pain in the past and do not wish to feel it again, they assume that during their rehabilitation, they will have to undergo discomfort. They catastrophize this expected pain, and begin to avoid any activities that could ultimately be helpful, such as coming to their physical therapy appointments.
The fear avoidance model is understandable, but its cycle can wind up with devastating consequences. Without physical therapy interventions, the patient is left in a state of muscle atrophy, disability and, often, depression. As these conditions worsen, the threat of pain gets closer and closer, and the cycle tightens. The way to avoid getting stuck in the fear avoidance model is to eliminate the fear of pain during rehabilitation. That’s where an aquatic environment comes into play.
How Post-Op In The Water Stops the Fear Avoidance Cycle
Mental optimism is a key to successful post-operative rehabilitation. Patient positivity can be buoyed by getting aquatic therapy as early as four days or a week after orthopedic surgery. The water is tremendously helpful because it offers several well-documented advantages over land-based physical therapy:
- Comfort. Aquatic therapy in a warm water environment, such as a specialized therapy pool, is comforting to the human body. This helps alleviate feelings of pain by naturally soothing aching muscles and joints.
- Support. In the water, a person’s land weight can be offset by up to 80 percent, depending upon the water depth. This provides support by taking weight off of affected joints/muscles and removes any anxiety related to falling.
- Swelling Reduction. Swelling, or edema, is a common occurrence post-surgery. Water compresses all the body surfaces, which improves circulation and reduces the condition of swelling.
- Faster Progression. While water is soothing, it is also invigorating and actually forces patients to work against its compression and resistance. This promotes faster progression after surgical procedures, which helps lift the spirits of patients who see improvement.
- Reduced Discomfort. Many patients have reported less discomfort during aquatic exercising. Their lowered perceived level of pain contributes to a desire to keep coming for their appointments, and pushing themselves to meet physical therapy goals.
In addition to these benefits, early intervention in the water can support greater joint range of motion (ROM) in the short and long-term. Limited ROM can lead to drop-off rates for adults who are disheartened by their progress; however, increasing ROM can be seen as a harbinger of excellent post-op results and a return to more normal activities of daily living. As noted in a study from Australia, two of the trials that were used for the meta-analysis indicated significant differences in ROM between the group that received early aquatic therapy and the group that receive later traditional, land-based therapy. The aquatic therapy patients were able to enjoy pain-reduced freedom of motion in their joints post-op, which translated to more comfortable, dependable movement during everyday life. Aquatic therapy and early ROM intervention only helps to encourage clients to continue with their treatment after undergoing a surgical procedure.
Safely Treating Patients Post-Op in the Water
The biggest concern from the view of most physicians is allowing patients who have recently had operations to get into water. The worry stems from the possibility of the wound becoming infected. However, proper wound waterproofing techniques enable physical therapy professionals to get their patients into water faster without contamination of the wound.
After the wound is no longer draining, water therapy can begin. As you can see in the video below courtesy of Randy Cohen, the first step is ensuring that the wound is completely covered in an occlusive waterproof dressing placed above a gauze pad. The gauze serves the purpose of providing physical proof that no water seeped into the dressing during the aquatic therapy session. By systematically focusing on completely sealing the wound area, physical therapists can ensure that their patients are water-ready.
The support for safe waterproofing during early post-op aquatic therapy sessions comes from studies and documentation like “Early Aquatic Physical Therapy Improves Function and Does Not Increase Risk of Wound-Related Adverse Events for Adults After Orthopedic Surgery: A Systematic Review and Meta-Analysis” from the Archives of Physical Medicine and Rehabilitation. During this research involving 287 participants who engaged in aquatic therapy as early as one week post-op, none of them experienced wound-related adverse events that were any different from those expected with land-based therapy. Thus, the study concluded that aquatic therapy could be safely used during the early stages after orthopedic surgery, especially to improve the activities of daily living on land.
Removing the Psychological Walls to Successful Early Post-Op Outcomes
When pain becomes less of a factor during physical therapy, patients and their physical therapists gain the benefits. Treatment happens on a much more consistent level, and individuals are less resistant to performing exercises to become stronger, more flexible and more stable. Additionally, early ROM can set the stage for positive feedback thanks to faster return to regular functional activities without fear of pain. Whenever this kind of optimistic feedback loop can be imprinted on clients, they and their physical therapists are in a position to make faster strides toward successful post-operative outcomes.
Offering aquatic therapy as early as safely possible to post-op patients can be one way to break through the fear-avoidance model and build resilience. When a positive foundation can be set, amazing achievements are possible. It all begins with the right mix of optimism and expertise, as well as the aquatic tools necessary to promote healing.